Covering nearly 2 m², the skin is the body’s largest, most visible organ and, as such, is essential for health. Not only does healthy skin retain water, regulate temperature, and detect gentle touch and pain via nerve endings, but it also acts as the main barrier against bacteria, viruses, fungi, and other foreign substances.
Because skin features like color, texture, wrinkles, shadows, and beauty marks differentiate people and shape identity, any change in appearance, due to age or other factors, can affect both physical and mental health and strongly affect confidence and self-esteem.
This article explores the structure and functions of the skin. It deep dives into the three-layered structure: the epidermis, dermis, and hypodermis, and examines how these layers work together and why they matter for skin health.
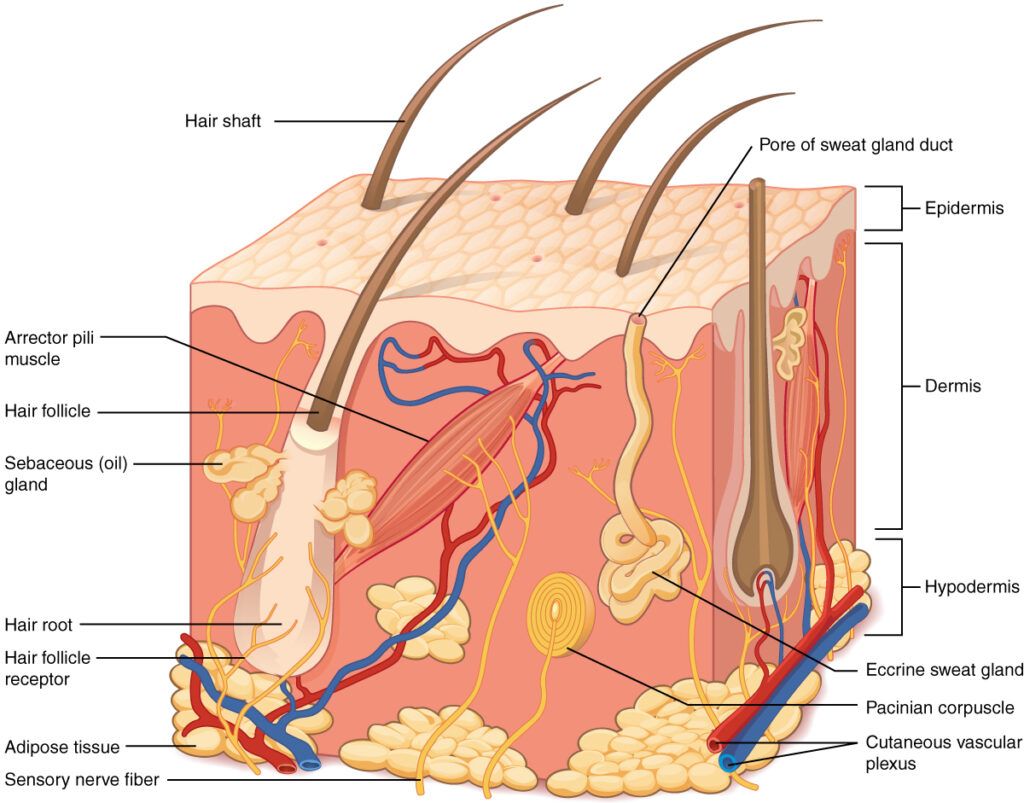
The skin structure: a multi-layered organ
The skin is a complex and dynamic organ with three main layers: epidermis, dermis, and hypodermis. Each has several sublayers composed of skin cells and skin appendages, such as hair follicles, sweat glands, and sebaceous glands, which perform different functions.
The epidermis: a major shield
The epidermis is the outermost layer of the skin, the part that is visible and touchable. It protects the body from toxins and bacteria while preventing fluid loss. Despite its thinness, it provides resistance and shields vital organs, muscles, nerves, and blood vessels from damage.
In most areas of the body, the epidermis measures approximately 0.1 mm in thickness. It is thinnest around the eyes (0.05 mm) and thickest on the soles of the feet (between 1 and 5 mm).
The epidermis is composed primarily of keratinocytes, which are continuously replenished and shed skin cells.
Keratinocytes are produced in the stratum basale (basal layer) and migrate toward the skin surface, where they die and are shed, subsequently replaced by newer cells.
During migration, keratinocytes mature and undergo several changes. This process, known as keratinization or cornification, defines the five distinct sublayers of the epidermis:
- Stratum basale (basal layer)
- Stratum spinosum (spinous layer)
- Stratum granulosum (granular layer)
- Stratum lucidum (clear layer)
- Stratum corneum (corneal layer)
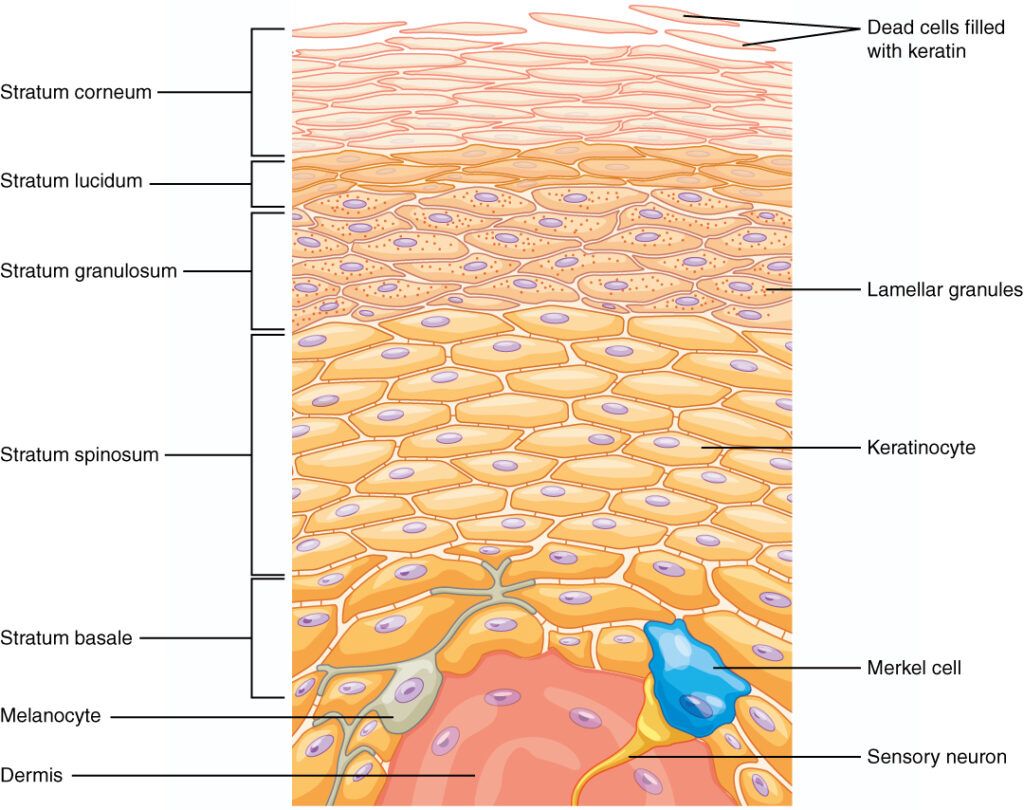
1. Stratum basale (basal layer)
The stratum basale is the deepest layer of the epidermis, consisting of a single layer of basal cells from which keratinocytes are produced and begin their migration.
Two additional cell types are present in the stratum basale:
- Melanocytes: These cells produce melanin, a pigment that determines skin and hair color. Melanin primarily filters UV radiation, thereby protecting DNA from damage and reducing the risk of harmful effects, such as skin cancer.
- Merkel cells: They function as receptors, stimulating sensory nerves that the brain perceives as touch. Merkel cells are the most abundant in the palms of the hands and soles of the feet.
2. Stratum spinosum (spinous layer)
The stratum spinosum consists of eight to ten layers of keratinocytes, formed through cell division in the stratum basale. Within this sub-layer, keratinocytes begin synthesizing keratin, a protein that binds cells together, and change to a spindle shape. They also release a water-repelling glycolipid, which helps prevent water loss and contributes to the skin’s relative waterproofness.
Langerhans cells are interspersed among the keratinocytes in this layer. These cells detect and engulf foreign substances, defending the organism against infections and contributing to cutaneous allergic reactions.
As new keratinocytes are produced in the stratum basale, existing keratinocytes in the stratum spinosum are pushed into the stratum granulosum.
3. Stratum granulosum (granular layer)
The stratum granulosum has a grainy appearance due to changes in keratinocytes as they are pushed from the stratum spinosum. In this layer, the cells become flatter, their membranes thicken, and they produce large quantities of keratin and keratohyalin. These proteins constitute the majority of the keratinocyte mass in this layer and are responsible for its grainy texture.
5. Stratum lucidum (lucid layer)
The stratum lucidum is a smooth, translucent layer of the epidermis found exclusively in the thick skin of the palms, soles, and digits. In this layer, keratinocytes are dead, flattened, and indistinguishable from one another. These cells are densely packed with eleiden, a clear, lipid-rich protein derived from keratohyalin, which imparts transparency and serves as a barrier to water.
5. Stratum corneum (corneal layer)
The stratum corneum is the outermost sublayer of the epidermis and is directly exposed to the external environment. It consists of 15 to 30 layers of flattened, dead cells, varying across body regions. These cells are bound by epidermal lipids, which are essential for skin health. The lipids form a protective barrier that prevents microbial penetration and dehydration of underlying tissues and provides mechanical protection against abrasion. A deficit in these lipids can result in dry, irritated, and rough skin.
The skin sheds dead cells from the stratum corneum through a process called desquamation, which occurs over approximately 4 weeks. The pores of sweat glands and the openings of sebaceous glands are also located within this layer.
Above the surface: the hydrolipid layer
The epidermis is covered by a hydrolipid layer—a serum of water and lipids—continuously renewed by sebaceous and sweat gland secretions. This serum maintains suppleness and serves as an additional barrier against microorganisms.
The aqueous component of this serum, referred to as the protective acid mantle, contains:
- Lactic acid and various amino acids, derived from perspiration.
- Free fatty acids, originating from sebum.
- Amino acids, pyrrolidone carboxylic acid, and other natural moisturizing factors (NMFs), primarily byproducts of the keratinization process.
The protective acid mantle imparts a slightly acidic pH to the skin (between 5.4 and 5.9), creating an optimal environment for:
- Beneficial microorganisms (skin microbiome) thrive and help eliminate harmful organisms.
- The formation of epidermal lipids.
- Enzymes that enable the desquamation process.
- The stratum corneum and its capacity to repair itself following damage.
The dermis: elasticity, support, and nutrition
The dermis constitutes the primary and thickest layer of the skin. It contains blood and lymphatic vessels, nerves, and additional structures, including hair follicles and sweat glands. The dermis is composed of two layers of connective tissue:
- The stratum reticulare (reticular layer)
- The stratum papillare (papillary layer)
1. Stratum reticulare (reticular layer)
The reticular layer is made of dense, irregular connective tissue. Its network of blood vessels and nerves supports the skin’s strength and flexibility. Elastin fibers provide elasticity for movement, while collagen fibers offer firm support, extending into the papillary layer and hypodermis. Collagen also helps retain moisture, supporting skin hydration.
2. Stratum papillare (papillary layer)
The papillary layer is composed of areolar connective tissue, characterized by a loosely organized mesh of collagen and elastin fibers. This superficial dermal layer projects into the stratum basale of the epidermis, forming finger-like dermal papillae.
The papillary layer contains fibroblasts, a small number of adipocytes, and numerous small blood vessels. It also houses phagocytes, which defend against bacteria and other pathogens that penetrate the skin. Additionally, this layer contains lymphatic capillaries, nerve fibers, and tactile receptors known as Meissner corpuscles.
Lifestyle and environmental factors, including sun exposure and temperature fluctuations, influence elastin and collagen levels and the composition of the extracellular matrix. With aging, the natural production of collagen and elastin decreases, reducing the skin’s water retention capacity. As a result, the skin loses firmness and wrinkles develop.
The Functions of the Dermis
The dermis protects the body through its thick structure, its capacity to nourish the outer skin layers, its role in waste elimination, and its involvement in thermoregulation via sweating.
- The firm, thick dermal structure cushions external impacts. In the event of injury, connective tissue components such as fibroblasts and mast cells facilitate tissue repair.
- The dermis contains numerous blood vessels that supply nutrients to the epidermis and assist in the removal of metabolic waste products.
- The dermis also houses sebaceous glands, which secrete sebum, and sweat glands, which release water and lactic acid onto the skin’s surface. These secretions collectively form the hydrolipidic film.
The hypodermis: energy storage and tissue connection
The hypodermis, or subcutaneous layer, is the deepest part of the skin. It contains well-vascularized, loose areolar connective tissue and adipose tissue.
It consists of the following components:
- Adipose cells (adipocytes): Fat-storing cells grouped in fibrous clusters.
- Special collagen fibers (septa): Spongy, loose connective tissue holding fat cells together.
- Blood vessels: Supply nutrients and oxygen to the hypodermis.
The thickness of the hypodermis varies: from only a few millimeters near the eyelids, to several centimeters thick in places such as the buttocks and abdomen, and can be hard to distinguish from the dermis.
The Functions of the Hypodermis
The primary function of the hypodermis is to connect the skin to the underlying fascia covering bones and muscles. But it also stores fat, insulates to reduce heat loss, provides a protective cushioning layer, and serves as an energy reserve.
Fat accumulation in the hypodermis is influenced by hormones. These include testosterone, estrogen, insulin, glucagon, and leptin, as well as genetic factors. Fat distribution changes with age. Men usually store fat in the neck, arms, lower back, and abdomen. Women tend to accumulate fat in the breasts, hips, thighs, and buttocks.
The Functions of the Skin
Healthy skin forms a protective barrier between the body and the external environment.
The first line of defense is the stratum corneum, the skin’s outermost layer, and acts against cold, heat, dehydration, and UV radiation.
The outer skin layer contains natural moisturizing factors, such as lactic acid and urea, derived from lipids. These substances help retain water, keeping the skin elastic, firm, and soft. When these factors decrease, the skin loses moisture and becomes rough, dry, and may chap.
Each skin layer plays a specific role in maintaining the skin’s protective barrier:
- Against temperature changes: Fat cells in the hypodermis insulate the body from cold and heat.
- Against pressure, shocks, and scratches: the epidermis is the first line of defense. The fat cells in the hypodermis create a protective layer that absorbs shocks, shielding the muscle tissue and fascia beneath.
- Against bacteria and viruses: the stratum corneum of the epidermis, along with its protective acid mantle, forms a barrier. If an element penetrates this first line of defense, the skin’s immune system responds.
- Against chemical substances: The hydrolipidic film and acid mantle help protect the body from harmful alkaline chemicals.
But that is not all; The skin also takes on many roles to support overall health and well-being:
- Temperature regulation: It cools the body through sweating and conserves heat by narrowing blood vessels in the dermis.
- Sensory control: Nerve endings in the skin detect pressure, vibration, touch, pain, and temperature. These senses influence behavior and help protect us from danger.
- Regeneration and repair: The skin, aided by its lipid content, regenerates itself and can heal wounds.
- Energy source: Adipose cells in the hypodermis store nutrients. When needed, these nutrients travel through blood vessels to organs such as the liver and brain.
- Psychological role: The skin serves as an interface with the external environment. Its appearance influences how people perceive each other. Healthy, well-functioning skin can enhance confidence and well-being.
The skin evolves continuously, from birth to death, especially as its water-retention capacity decreases. But it also evolves in reaction to lifestyle. For example:
- With regular UV exposure, melanin production increases, the skin thickens to protect itself, and dark spots may develop.
- When exposed to repeated friction, the skin’s outer layer thickens. For example, calluses form on the hands or feet from ongoing rubbing.
To conclude
The skin is a complex organ composed of layers that collaborate to protect the body and maintain balance. The epidermis acts as a protective barrier, the dermis offers strength and elasticity, and the hypodermis supports and stores energy.
Understanding this architecture is essential for evaluating how cosmetic and dermatologic products function. Knowledge of skin structure allows us to identify its needs and select the most effective products.
Sources
- https://www.frontiersin.org/journals/pharmacology/articles/10.3389/fphar.2020.00785/full?utm_source=chatgpt.com
- https://www.eucerin.fr/a-propos-de-la-peau/comprendre-la-peau/structure-et-fonction-de-la-peau
- https://www.msdmanuals.com/fr/accueil/troubles-cutan%C3%A9s/biologie-de-la-peau/structure-et-fonction-de-la-peau
- https://pressbooks-dev.oer.hawaii.edu/anatomyandphysiology/chapter/layers-of-the-skin/

