Sun exposure is a primary cause of skin damage. Although it is necessary for vitamin D synthesis, ultraviolet (UV) radiation is the main external factor responsible for both immediate and long-term skin changes.
Beyond sunburn, repeated UV exposure leads to cumulative damage, accelerates photoaging, and increases the risk of skin cancer. Lifetime UV exposure is strongly associated with non-melanoma skin cancers, while intense, intermittent exposure, particularly sunburn, raises melanoma risk.
Understanding these effects is vital for public health and for cosmetic brands developing protective and reparative products. This article reviews acute, chronic, and precancerous skin lesions caused by UV radiation, highlighting key biological mechanisms and visible outcomes.
Acute Damage: Tanning, Sunburn, and Photosensitivity
Tanning
Tanning is a visible response to UV exposure. When skin encounters ultraviolet radiation, melanocytes increase melanin production to absorb UV energy. This darkening offers limited photoprotection but indicates existing skin damage. Even a slight tan signals DNA stress and activates defense mechanisms. Although tanning may be considered attractive, it does not prevent cumulative UV damage, premature aging, or increased cancer risk.
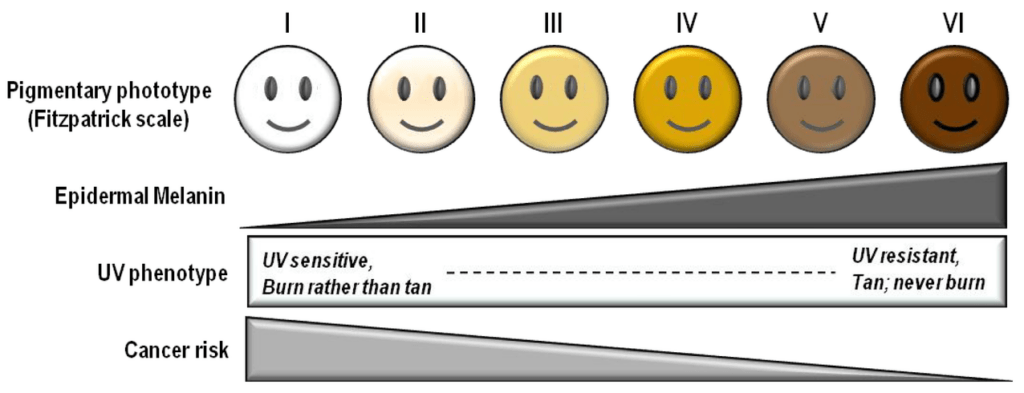
The tanning response varies by phototype, age, and previous sun exposure. Fair-skinned individuals with less melanin have minimal protection and are especially vulnerable to UV effects. While darker skin provides more natural defense, cumulative damage and photoaging still occur over time.
Sunburn
Sunburn is an acute skin inflammation primarily caused by UVB radiation. It typically results in redness, swelling, and pain, and can progress to blistering, fever, and chills in severe cases. Symptoms develop within 12 to 36 hours of exposure and are often followed by skin peeling.
Note: repeated sunburns in childhood and adolescence significantly increase the risk of melanoma later in life.
A sunburn occurs when UVB radiation damages DNA in keratinocytes, causing inflammation and attracting immune cells. This results in vasodilation, redness, and swelling. Oxidative stress from free radicals further increases tissue damage. These effects highlight the need for antioxidant defenses and DNA repair to maintain skin resilience.
The amount of UV exposure required to induce sunburn depends on both individual and environmental factors. Melanin content serves as a primary determinant, as it contributes to the skin’s natural photoprotective capacity. Aging increases susceptibility to sunburn by reducing melanocyte activity and decreasing tanning efficiency. And environmental factors include time of day, latitude, altitude, and cloud cover, etc.
Photosensitivity
Photosensitivity refers to acute reactions triggered by UV exposure, including solar urticaria, chemical photosensitivity, and polymorphic light eruption. These conditions are marked by erythema, itchiness, and sometimes blistering.
Solar urticaria develops within minutes of sun exposure and can last from a few minutes to several hours. Severe cases may include systemic symptoms such as headaches, weakness, or nausea.
Chemical photosensitivity occurs when UV radiation interacts with certain chemicals, medications, or plant compounds, resulting in phototoxicity or photoallergy. Phototoxic reactions resemble sunburn and are limited to sun-exposed areas, while photoallergic reactions involve immune responses and can sometimes affect non-exposed skin. Substances such as sulfonamides, aftershaves, and some sunscreens may trigger photoallergy, which usually appears 24 to 72 hours after exposure.
Polymorphic light eruption is common but not well understood. It appears as erythema, nodules, or vesicles with intense itching, mainly on sun-exposed areas such as the neck, upper chest, arms, or backs of the hands. Repeated exposure can lead to skin hardening and reduced sensitivity to sunlight.
Chronic Effects: Photoaging and Skin Alterations
Chronic UV exposure leads to photoaging, a progressive and largely irreversible process. Both UVA and UVB radiation accelerate the development of fine lines, deep wrinkles, irregular pigmentation, lentigines, yellowish discoloration, and a roughened texture. Photoaged skin gradually loses elasticity and suppleness, reducing its youthful appearance.
At the cellular level, UVA penetrates deeply into the dermis and impairs fibroblast function, reducing collagen and elastin production. Loss of these proteins decreases skin firmness and promotes the formation of wrinkles. In the epidermis, Keratinocytes and melanocytes are also stimulated to produce melanin and inflammatory mediators, leading to hyperpigmentation and uneven tone.
All skin types are susceptible, though fair skin is more prone to visible signs of photoaging. Cosmetic interventions such as chemical peels, alpha-hydroxy acids, tretinoin creams, and laser resurfacing can improve superficial signs, such as uneven pigmentation or fine lines, but are less effective for deep wrinkles or extensive structural damage.
UV exposure also alters the skin microbiome, changing bacterial and fungal populations. Disruption of this balance can weaken barrier function, increase inflammation, and reduce the skin’s ability to respond to environmental stressors. Maintaining or restoring a healthy microbiome presents a promising opportunity for skincare innovation.
Cumulative exposure is critical. Decades of sun exposure gradually compromise the skin barrier, deplete antioxidants, and reduce DNA repair efficiency, increasing vulnerability to long-term damage.
Precancerous Lesions and Skin Cancers
Actinic Keratoses
Actinic keratoses (AK) are rough, scaly patches that develop after prolonged sun exposure and are considered precancerous. They are usually pink or red, though gray or brown variations can occur. AKs should be distinguished from seborrheic keratoses, which are benign growths that may appear on unexposed skin.
AK prevalence increases with age, cumulative UV exposure, and certain phototypes. Some lesions may regress, but others can progress to squamous cell carcinoma. Individuals with fair skin, light hair, blue eyes, advanced age, or immunodeficiency are at the highest risk.
Skin Cancer
UV radiation is the primary cause of skin cancer, the most common cancer in fair-skinned populations. Risk factors include genetic predisposition (skin type, number of moles, family history) and acquired factors (immunosuppression, cumulative UV exposure, sunburn history). The main types of skin cancer are:
- Basal cell carcinoma (BCC): Originates from epithelial cells, typically on sun-exposed areas. BCC grows slowly, rarely metastasizes, but can cause local tissue destruction.
- Squamous cell carcinoma (SCC): Usually arises from actinic keratoses and appears as thick, scaly patches. SCC can metastasize if untreated, posing a greater risk than BCC.
- Melanoma: Arising from melanocytes, melanoma is the most lethal skin cancer. It can develop de novo or from existing moles, often showing irregular borders and uneven pigmentation. Early detection is crucial, as untreated melanoma may progress rapidly and metastasize. Intermittent intense UV exposure, especially severe sunburns during youth, is strongly associated with melanoma risk.
To conclude
Sun exposure causes a wide range of skin damage, including acute effects such as tanning, sunburn, and photosensitivity, as well as long-term effects such as photoaging, precancerous lesions, and skin cancer. While the skin has natural defenses, including melanin, antioxidants, and DNA repair mechanisms, these are insufficient to fully prevent cumulative UV damage.
Understanding biological responses such as barrier disruption, oxidative stress, and microbiome imbalance allows cosmetic brands to develop products that enhance skin defenses, support repair, and promote long-term resilience.
Sources
- https://www.msdmanuals.com/fr/accueil/troubles-cutan%C3%A9s/l%C3%A9sions-cutan%C3%A9es-dues-au-soleil/coups-de-soleil
- https://www.sciencedirect.com/science/article/abs/pii/S0738081X10001628
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9971785
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12018068/https://www.who.int/fr/news-room/questions-and-answers/item/radiation-the-known-health-effects-of-ultraviolet-radiation

